Optimizing Your Glucose
Resources and tools for success using
a Continuous Glucose Monitor.

How to Use a Continuous Glucose Monitor
A Continuous Glucose Monitor (CGM) serves as an advanced tool for tracking blood sugar levels in real-time, eliminating the need for frequent finger pricks associated with traditional glucometers. Its continuous monitoring capabilities offer invaluable insights into blood glucose patterns and trends. This information aims to streamline the process of initiating CGM usage.

Before You Start
Other Considerations Before Wearing a CGM
> It is helpful to apply the sensor when your blood glucose is stable. Plan to apply the sensor when your blood sugar will be stable for the warm-up phase of the sensor. In general, wait 2 hours after a meal, 1 hour after moderate or intense activities, and 90 minutes after an insulin dose.
> It is not recommended to use a CGM if critically ill or on dialysis.
> The sensor will need to be removed prior to any imaging (MRI, CT, or X-rays) as these devices may affect the accuracy of the readings.
> Avoid prolonged exposure to extreme temperatures (below 36F and above 82F) or submerging in water for more than 30 minutes.
> Intense exercise may cause the sensor to loosen due to sweat or movement. This can lead to inaccurate or unreliable readings. If necessary, use specially designed patches or bands to secure the sensor onto your arm or use a medical adhesive to ensure a more secure fit.
> Do not block the hole on the sensor with an impermeable patch or band as it can cause moisture from sweat or other sources to accumulate and loosen the sensor from your skin.
> For optimal monitoring, ensure your monitoring device remains charged and within range of your sensor. If this isn't possible, reconnect the sensor to the device as soon as possible to maintain an accurate tracking history.
Tips for Traveling with a CGM
> Bring an extra sensor in case the one you are wearing needs to be replaced due to unexpected malfunction or it falls off.
> If travelling by airplane, it is recommended to ask for alternative screening methods for yourself or your luggage as the X-ray scanners and body image machines at airports may affect the accuracy of the readings. Airport metal detectors (walk-through and wand) will not affect the sensor.
Activating Sensor & App Set-Up

Validate your sensor any time your symptoms don't match an alarm.
Adjusting Your Sensor's Settings
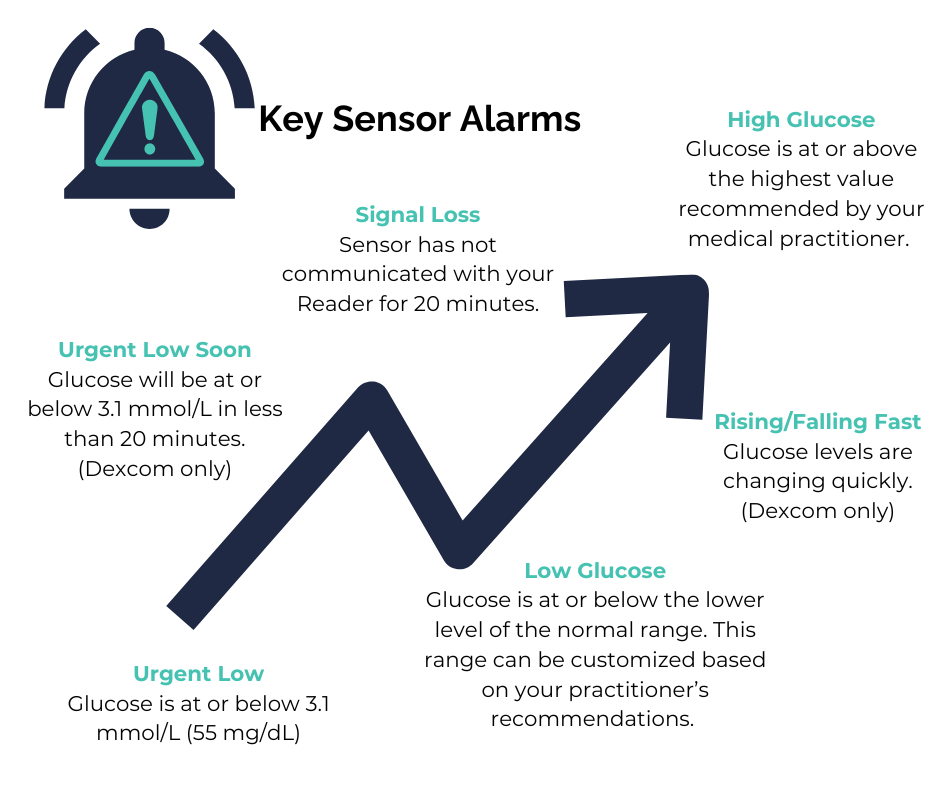
Understanding Your Sensor Readings
Two key concepts to understand: Current Glucose and the Trend Arrow.
Current Glucose
Your CGM displays the most recent glucose reading from interstitial fluid, the fluid between your skin and blood vessels, which may differ from a glucometer reading when blood glucose is changing rapidly.
Imagine it as a train with the engine representing the blood glucose value (BG) and the sensor glucose value (SG) as the caboose. After meals, BG rises before SG. Conversely, after meals, SG may remain higher until BG stabilizes.
If you doubt your sensor reading, use a glucometer for confirmation before making treatment decisions. Remember, during the first day of using a CGM, use a glucometer to validate the readings from your sensor and to make any treatment decisions.

Trend Arrows
Knowing your current blood glucose value is important. It is also important to know which direction your blood sugar is trending. The angle and direction of the trend arrow indicates stability, increases, or decreases in glucose levels and will impact the decisions you make regarding meals and treatments.
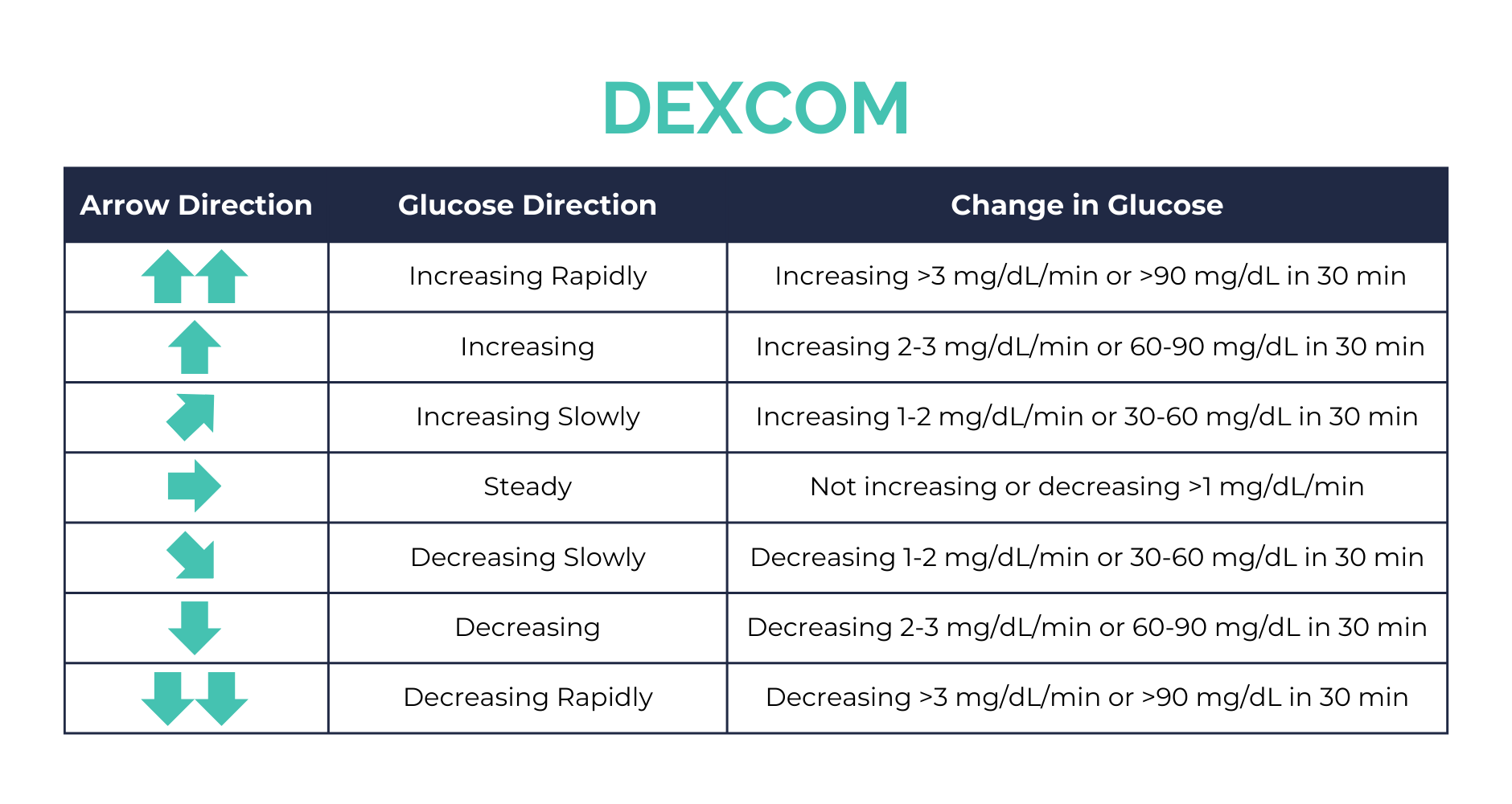

Understanding & Making Treatment Decisions
What Causes Changes in Blood Sugar Levels?
Blood glucose levels change due to diet, meal frequency, activity, and stress. All these influences need to be considered when making treatment decisions and when learning about how your body responds to them. For better insight of how your body responds to blood sugar, use your device to track meals, activity, insulin, and stressful events.
Rapid rises beyond the ideal range are spikes, while rapid drops are crashes. Aim to keep glucose within the ideal range a majority of the time. Consult your healthcare provider for personalized management recommendations.

Symptoms of High or Low Blood Sugar
It is important to understand the symptoms of low (hypoglycemia) and high (hyperglycemia) blood sugar while using a CGM. If your symptoms do not match the sensor’s reading, use a glucometer to double check the sensor accuracy and/or consult your health care professional.


Useful Links
ABBOTT FREESTYLE
Freestyle Libre 2
Phone Compatibility
User Guide
How to Videos
Support
Freestyle Libre 3

